RI has highest antibiotic use in New England
And that matters to you because….? Well, because if the bacterial infection you’re suffering from has evolved a resistance to available antibiotics, it will be harder to treat. There’s some new data about the spread of resistance, and new attention on it today.
The CDC is promoting its “Get Smart About Antibiotics Week,” and the Center for Disease Dynamics, Economics, and Policy has just updated its “ResistanceMap,” which shows where the resistance hot spots are in the U.S. and internationally.
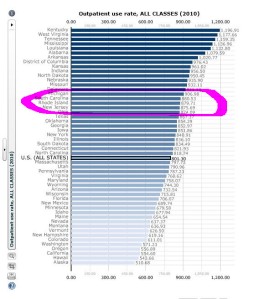
(About the graphic: this is a smallish screenshot of the CDDEP’s state-by-state resistance data on which I’ve circled Rhode Island. Click on it for a larger view. And you can see the original here.)
Here’s some background on the problem from the CDDEP:
Scientists have been aware of antibiotic resistance since shortly after the discovery of penicillin, western medicine’s first antibiotic. To a certain extent resistance is inevitable—as we use an antibiotic over time, resistance to the drug gradually evolves, making infections more difficult to treat and necessitating new and more powerful drugs. However, the development of resistance is also impacted by our actions—for example by how often we prescribe and use antibiotics, and how well we control and prevent infections acquired in the hospital. In order to design sensible solutions that prolong the useful life of antibiotics, policymakers need to be able to provide factual evidence, identify trends and measure the scope of the resistance problem.

Trackbacks